Pfizer, Moderna COVID-19 vaccines likely offer long-lasting protection, study finds
ST. LOUIS - The Pfizer-BioNTech and Moderna COVID-19 vaccines generate an immune response that is both strong and potentially long-lasting, according to new research.
A study published Monday in the journal Nature found evidence that the vaccines induced strong, persistent immunity to COVID-19. The evidence suggests that many who have already received either vaccine may not need a booster shot, as long as the coronavirus and its variants do not significantly evolve and render the vaccines ineffective.
Both Pfizer and Moderna vaccines were developed with mRNA technology, which provides instructions for the body to build and release foreign proteins, such as the spike protein found in SARS-CoV-2, the virus that causes COVID-19.
The new study, led by researchers at Washington University School of Medicine in St. Louis, found that immune cells were still being churned out to fight the virus nearly four months after receiving the first dose.
The team focused on the so-called germinal centers in the lymph nodes. Germinal centers, which form either from natural infection or vaccination, are like "boot camps for immune cells" where inexperienced cells are trained to better recognize the enemy and sharpen weapons, according to the university.
"We found that germinal centers were still going strong 15 weeks after the vaccine’s first dose," said senior study author Ali Ellebedy, PhD, an associate professor of pathology & immunology at Washington University. "We’re still monitoring the germinal centers, and they’re not declining; in some people, they’re still ongoing. This is truly remarkable."
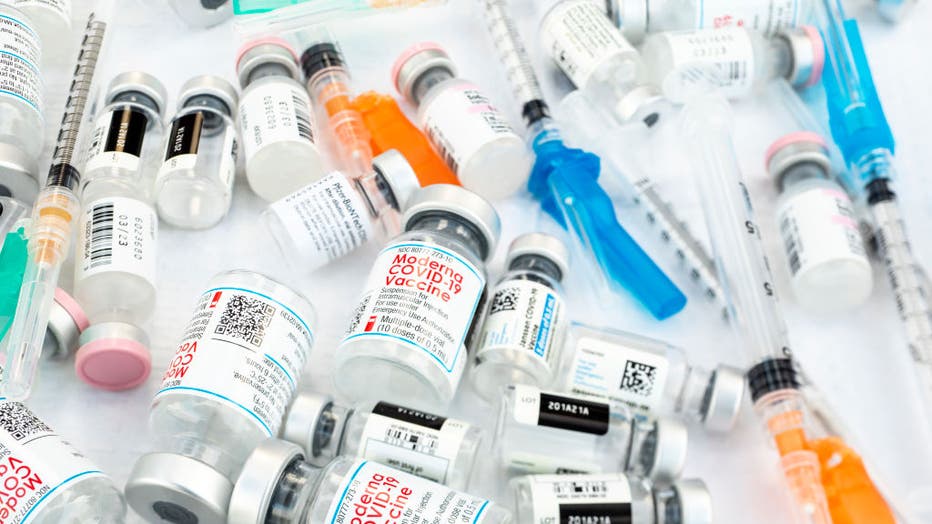
FILE - Bottles of the three current COVID-19 vaccines from Johnson & Johnson, Moderna and Pfizer-BioNTech are photographed at the COVID-19 vaccination site at Kedren Community Health Center on May 13, 2021, in Los Angeles, California. (Jay L. Cle
Scientists don’t fully understand why some vaccines induce protection that lasts a lifetime, such as the one for smallpox, while others require regular booster shots. But many have suspected that the difference may be due to the quality of the germinal centers brought on by different vaccines.
The Pfizer and Moderna vaccines received an emergency use authorization from the U.S. Food and Drug Administration in December. The mRNA vaccines, which stand for Messenger RNA vaccines, are new — but have been studied for decades.
Ellebedy and his team first began studying whether this new kind of vaccine induces a good germinal center response in mid-December. The study involved 41 participants, including eight who had been previously infected with the virus. All were immunized with two doses of the Pfizer-BioNTech vaccine.
Among 14 of these people, scientists extracted cells from the lymph nodes in the armpit at three, four, five and seven weeks after the first dose. Ten of the participants gave additional samples 15 weeks after the first dose. None of these 14 people had previously been infected with the virus.
The team found that all 14 participants had formed germinal centers with B cells producing antibodies that target a key SARS-CoV-2 protein. The response increased after the second shot and then stayed high, researchers said.
At 15 weeks after the first dose, eight of 10 people still had detectable germinal centers containing the B cells targeting the virus, according to the study.
"The fact that the reactions continued for almost four months after vaccination — that’s a very, very good sign," Ellebedy told the New York Times. He added that germinal centers typically peak one to two weeks after immunization and then diminish.
The team also obtained blood samples from all 41 people who received the Pfizer vaccine. Samples were obtained before the administration of each dose of the vaccine, as well as at weeks four, five, seven and 15 after the first dose.
In people who were not previously infected with the coronavirus, antibody levels increased slowly after the first dose and peaked one week after the second. People who previously had been infected already had antibodies in their blood before the first dose. Their levels quickly increased after the first dose and peaked higher than the uninfected participants’ levels, researchers said.
Dr. Jane O’Halloran, the co-first author of the study and Washington University assistant professor of medicine, said they didn’t aim to compare the effectiveness of vaccination in people with and without a history of infection — "but when we looked at the data we could see an effect."
"If you’ve already been infected and then you get vaccinated, you get a boost to your antibody levels. The vaccine clearly adds benefit, even in the context of prior infection, which is why we recommend that people who have had COVID-19 get the vaccine," O’Halloran said.
The study echoed previous findings reported in May that the immunity created after having COVID-19, in addition to getting vaccinated, could last in the body for years.
RELATED: Immunity to COVID-19 could last for years, new studies suggest
How long protection will last from the mRNA vaccines remains unknown. The study suggests that many of those who have received the Pfizer and Moderna vaccines will be protected over the long term against many of the existing coronavirus variants. The findings showed that vaccines produced high levels of neutralizing antibodies effective against three variants of the virus, including the one originally detected in South Africa that has shown some resistance to vaccines.
But experts say a booster may be needed as the virus continues to spread and evolve around the world in areas with low vaccination rates.
"Anything that would actually require a booster would be variant-based, not based on waning of immunity," Dr. Deepta Bhattacharya, an immunologist at the University of Arizona, told the Times. "I just don’t see that happening."
This story was reported from Cincinnati.


